Morphological characteristics of the duodenum by using imaging studies
Keywords:
enfermedades del duodeno, diagnóstico por imágenes, radiologíaAbstract
Background: the duodenum is the only segment of the intestine that presents a double location, in relation to the peritoneum, behaving as an intra and extra-peritoneal organ, contributing to determine a large number of diseases that occur from congenital anomalies, traumatic, inflammatory, even the neoplastic entities.
Objective: to describe the anatomical-clinical modifications of the duodenum, through imaging studies.
Methods: a cross-sectional descriptive study was carried out where the universe was constituted by 26 radiological reports of medical indications in contrasted esophageal, stomach and duodenum exams to patients with symptomatology in these organs. Subsequently, the radiological reports and data obtained were processed, showing the results in tables.
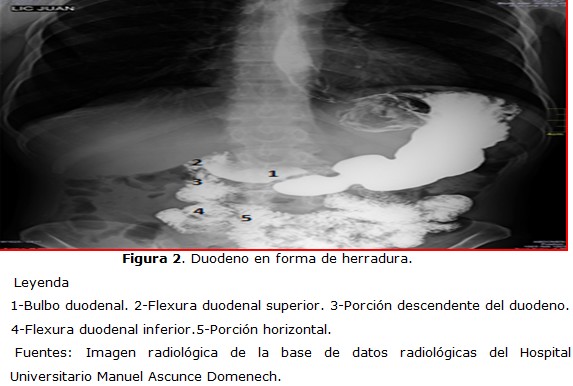
Results: in all cases, the situation, relations and portions of the duodenum were maintained. The forms of the duodenum found were: horseshoe and letter C, a predominance of the last. Most cases did not present clinical-radiological alterations, in the rest, a small number of entities: duodenal ulcer and widening of the duodenal frame.
Conclusions: a predominance in the form of letter C as a duodenal frame was observed. When relating these forms with the modifications and clinical entities, the horseshoe showed a greater number. The group of 61 to 70 years predominated at the expense of the male sex. In the study, more than half of the cases did not present clinical-radiological alterations and the frequency of the clinical-radiological entities showed the predominance of the duodenal ulcer and the widening of the duodenal frame.
DeCS: DUODENUM/anatomy&histology; DUODENUM/diagnostic imaging; DUODENAL ULCER/diagnostic imaging; AGED; MALE.
Downloads
References
1.Drake RL, Voge AW, Mitchell AWM. Gray anatomía para estudiantes. 2da Ed. Barcelona: Elsevier; 2010.
2.Moore KL, Dalley AF, Agur AMR. Abdomen. En: Moore KL, Dalley AF, Agur AMR, Editores. Moore anatomía con orientación clínica. 7ed. Philadelphia: Wolters Kluwer/ Lippincott Williams & Wilkins; 2013. p. 181-325.
3.Rouvière H, Delmas A. Abdomen. En: Rouvière H, Delmas A. Anatomía Humana descriptiva, topográfica y funcional. 10 ed. T2. Barcelona: Masson SA; 2002. p.316-379.
4.Castillo GL, González AV, Espinosa QD. Morfofisiología. 2 ed. T 3. La Habana: Ecimed; 2015.
5.Prives M, Lisenkov N, Bushkovich V. Derivados del intestino medio. En: Prives M, Lisenkov N, Bushkovich V, editores. Anatomía humana. 5 ed. T2. Moscú: Mir; 1989.p.64.
6.Sadler TW. Langman. Embriología médica con orientación clínica. 13. ed. Philadelphia: Wolters Kluwer; 2017.
7.Beltrán MA. Tumores del estroma gastrointestinal (gist) del duodeno: presentación clínica, estudio diagnóstico y tratamiento actual. Rev Chil Cir [Internet]. Ago 2014 [citado 13 Nov 2018];66(4):[aprox. 12 p.]. Disponible en: https://scielo.conicyt.cl/scielo.php?script=sci _arttext&pid=S0718-4026 2014000400016&lng=es
8.Yang F, Jin C, Du Z, Subedi S, Jiang Y, Li J, et al. Duodenal gastrointestinal stromal tumor: Clinicopathological characteristics, surgical outcomes, long term survival and predictors for adverse outcomes. Am J Surg [Internet]. 2013 [citado 13 Nov 2018];206(3):[aprox. 7 p.]. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/23673012
9.García Luna PP, López Gallardo G. Evaluación de la absorción y metabolismo intestinal. Nutr Hosp [Internet]. May 2007 [citado 13 Nov 2018];22(Suppl 2):[aprox. 8 p.]. Disponible en: http://scielo.isciii.es/pdf/nh/v22s2/fisiologia1.pdf
10.Rodriguez Olaso X, Olano Gossweiler C, Lopez Gonzalez V. Uso de nuevas técnicas y procedimientos endoscópicos en el diagnóstico y seguimiento de la enfermedad celíaca. Rev Urug Med Interna [Internet]. 2018 [citado 13 Nov 2018];(1):[aprox. 11 p.]. Disponible en: http://www.scielo.edu.uy/pdf/rumi/v3n1/2393-6797-rumi-3-01-3.pdf
11.Beham A, Schaefer IM, Cameron S, von Hammerstein K, Füzesi L, Ramadori G, et al. Duodenal GIST: a single center experience. Int J Colorectal Dis. 2013 Apr;28(4):581-90.
12.Agaimy A, Vassos N, Croner RS. Gastrointestinal manifestations of neurofibromatosis type 1 (Recklinghausen's disease): Clinicopathological spectrum with pathogenetic considerations. Int J Clin Exp Pathol [Internet]. 2012 [citado 13 Nov 2018];5(9):[aprox. 10 p.]. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3484498/.
13.Hernández HRG. Manual de Endoscopia digestiva superior diagnóstica. 2 ed. La Habana: Ciencias Médicas; 2014.
14.Gómez Zuleta MA. Ecoendoscopia en la evaluación de las lesiones subepiteliales duodenales. Rev Col Gastroenterol [Internet]. Jun 2015 [citado 13 Nov 2018];30(2):[aprox. 5 p.]. Disponible en: http://ww w.scielo.o rg.co/p df/rcg/v 30n2 /v3 0n2a09.pdf
15.Armstrong D, Barkun A, Bridges R, Carter R, de Gara Ch, Dubé C, et al. Canadian Association of Gastroenterology consensus guidelines on safety and quality indicators in endoscopy. Can J Gastroenterol [Internet]. 2012 Jan [citado 13 Nov 2018];26(1):[aprox. 14 p.]. Disponible en: https://www.ncbi.nlm.nih.gov/pubmed/22308578
16.Buscaglia J, Nagula S, Jayaraman V, Robbins D, et al. Diagnostic yield and safety of jumbo biopsy forceps in patients with subepithelial lesions of the upper and lower GI tract. Gastrointest Endosc [Internet]. 2012 [citado 13 Nov 2018];75:[aprox. 5 p.]. Disponible en: http://www.sci elo.org.co/sc ielo.php? script= sci_arttext&pid=S0120-9957 2016 000 300 014&lng=en
17.Larghi A, Fuccio L, Chiarello G, Attili F, Vanella G, Paliani GB, et al. Fine-needle tissue acquisition from subepithelial lesions using a forward-viewing linear echoendoscope: Endoscopy [Internet]. 2014 [citado 13 Nov 2018];46(1):[aprox. 6 p.]. Disponible en: http://www.sc ielo.org.co/s cielo.php?sc ript=sci_ arttext& pid=S0120-995 7201 6000 300014&lng=en
18.Hamada T, Yasunaga H, Nakai Y, Isayama H, Horiguchi H, Matsuda S, et al. Rarity of severe bleeding and perforation in endoscopic ultrasound-guided fine needle aspiration for submucosal tumors. Dig Dis Sci [Internet]. 2013 [citado 13 Nov 2018];58(9):[aprox. 4 p.]. Disponible en: http://www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0120-99572016 000300014&lng=en
19.Waisberg J, Joppert Netto G, Vasconcellos C, Sartini GH, Miranda LS, Franco MI. Carcinoid tumor of the duodenum: a rare tumor at an unusual site. Case series from a single institution. Arq Gastroenterol [Internet]. 2013 [citado 13 Nov 2018];50(1):[aprox. 6 p.]. Disponible en: http://www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0120-99572016 000300014&lng=en
20.Utku Yilmaz T, Kozan R. Duodenal and jejunal dieulafoy´s: optimal management. Clin Exp Gastroenterol [Internet]. 2017 [citado 13 Nov 2018];10: [aprox. 8 p.]. Disponible en: https://ww w.ncbi.n lm.nih.go v/pmc/articles/PMC5683779/.
21.Sinelnikov RD. Atlas de Anatomía Humana. T2. 4 ed. Moscú: Mir; 1979.
22.Latour Ramos R. Embriología, anatomía, histología y fisiología del estómago y duodeno. Paniagua Estévez ME, Piñol Jiménez FN. Gastroenterología y hepatología clínica. T.3. La Habana: Ciencias Médicas; 2015.
23.Rojas A, Carvajal GD, Prieto RG, Aponte DM. Lesión de Dieulafoy de duodeno: hallazgo inusual. Rev Col Gastroenterol [Internet]. 2016 Sep [citado 13 Nov 2018];31(3):[aprox. 4 p.]. Disponible en: http://www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0120-995 72016 00 0300014&lng=en
24.Córdova H, Sánchez-Montes C, Delgado-Guillena PG, Morales VJ, Sendino O, González Suárez B. Quality indicators for esophagogastroduodenoscopy: A comparative study of outcomes after an improvement programme in a tertiary hospital. Gastroenterol Hepatol [Internet]. 2017 Nov [citado 13 Nov 2018];40(9):[aprox. 7 p.]. Disponible en: https://www.ncbi.n lm.nih.gov/pubmed/28648767
25.Buils Vilalta F, Martínez Ramos D, Sánchez Cano JJ, Domenech Calvet J, Vives Espelta M, Socías Seco M, et al. Tratamiento laparosconpico de un paciente con diverticulitis yeyunal perforada. Rev Andaluza Patol Dig [Internet]. 2013 [citado 13 Nov 2018];36:[aprox. 3 p.]. Disponible en: https:// www.sapd.es/revista/2013/36/4/05
26.Parra Blanco A. Lesiones submucosas del tubo digestivo. Rev esp enferm dig [Internet]. 2012 Dic [citado 13 Nov 2018];104(11):[aprox. 1 p.]. Disponible en: http://scielo .isciii.es/sci elo.php?scri pt=sci_arttext&pid=S1130-01082012001100011&lng=es
27.Mohammed I, Wagholikar GD. Dieulafoy’s lesion of duodenum: a case report. BMC Gastroenterology [Internet]. 2003 [citado 13 Nov 2018];(3):[aprox. 12 p.]. Disponible en: https://w ww.ncbi. nlm.nih. gov/p mc/ articles/PMC149361/.